A semen analysis is a standard test to evaluate the quality and quantity of sperm. It’s often the first recommended test for male infertility and can provide valuable information for couples who are struggling to conceive.
Although this test may not offer a comprehensive view of a male’s overall fertility, it’s a good starting point, as an abnormal result can provide clues and narrow the scope of further testing.
This article explores what a semen analysis entails, how it’s performed, and what the results may indicate.
Semen analysis: An overview
Semen analysis is a diagnostic tool used to evaluate male fertility. It’s a simple and non-invasive procedure that involves sperm collection followed by laboratory testing. This section provides an overview of the test and its significance in assessing male infertility.
What is semen?
Semen is the substance released from the penis during ejaculation (orgasm).
It contains sperm and several other components, including:
- Sperm: These are male reproductive cells responsible for fertilizing an egg. Sperm have a unique shape that includes a head (genetic material) and a tail for mobility.
- Seminal fluid: This fluid allows sperm to travel through the female reproductive system and fertilize an egg. Seminal fluid contains a mixture of fluids from several glands, including the prostate gland and seminal vesicles.
- Proteins and enzymes: These substances fuel the sperm’s journey and protect them from the acidic environment of the female reproductive system.
Semen can also contain white blood cells, fructose, vitamin C, and zinc.
What is male infertility?
Infertility is a common problem that affects both men and women. Male infertility, in particular, affects one in every six couples trying to conceive. Moreover, nearly half of all infertility cases are due to male factor infertility.
What is Male Factor Infertility? | Explained by Dr. Jacqueline Gutmann
Male infertility is the inability to achieve pregnancy after a year or more of regular, unprotected sex.
Possible causes of male infertility include, but are not limited to:
- Low sperm count or poor sperm motility: There are too few sperm, or the sperm are not moving properly, making it difficult to reach and fertilize an egg.
- Varicocele (swelling of the veins in the scrotum): Varicoceles are very common and can lead to a variety of abnormal semen analysis parameters, including; low sperm count, decreased sperm motility, and abnormal sperm morphology (shape).
- Hormonal imbalance: Hormonal imbalances, such as low testosterone levels, can affect sperm production and lead to infertility.
- Erectile dysfunction: Erectile dysfunction is a condition that makes it difficult or impossible to achieve or maintain an erection.
- Retrograde ejaculation: In this condition, semen is released into the bladder instead of being ejaculated out of the penis, which can cause infertility.
- Blockages in the reproductive tract: Blockages can prevent sperm from being released during ejaculation.
- Genetic disorders: Certain genetic disorders, such as Klinefelter syndrome or Cystic Fibrosis, can cause infertility in men.
- Trauma to the testicles: Previous injury to the testicles may affect sperm production and cause infertility.
- Cancer treatment: Cancer treatments, such as chemotherapy, radiation therapy, and surgery, can damage the reproductive system and lead to infertility.
- Lifestyle choices: Smoking, heavy alcohol use, drug use, anabolic steroid use, and obesity can also contribute to male infertility.
- Exposure to toxins: Exposure to toxins, such as pesticides, lead, and radiation, can damage sperm and affect fertility.
It’s important to note that this isn’t an extensive list of causes for male infertility. Male infertility is a complex condition that can have multiple underlying causes.
Struggling to Conceive? This Guide Changes Everything
Discover the expert strategies to finally start your family—download your free guide by Dr. Marcy Maguire now!

What is a semen analysis?
A semen analysis is a laboratory test that evaluates the quality and quantity of an individual’s semen. It’s a non-invasive and straightforward procedure that involves collecting a semen sample and examining it under a microscope. This test can provide valuable information about a man’s fertility status, including his sperm count, motility, and morphology.
Who needs a semen analysis?
Semen analysis is typically recommended for couples trying to conceive for at least one year without success (or six months if the female partner is 35 years old or older). If male infertility is suspected, and the female partner has already undergone fertility testing, a semen analysis is usually the next step in diagnosing the cause of infertility.
A semen analysis may be recommended for men with certain medical conditions or lifestyle factors that can affect their fertility, such as a history of testicular cancer, previous chemotherapy or radiation treatment, or exposure to toxins in the workplace. In some cases, a semen analysis may be part of routine testing for men who are considering donating sperm or for those who are undergoing fertility treatments such as in vitro fertilization (IVF).
The Semen Analysis Procedure
This section covers the procedure, including the steps before, during, and after the test.
What happens during a semen analysis?
During a semen analysis, the patient must provide a semen sample either by ejaculating into a sterile container in a private room at a fertility clinic or by using a special condom during intercourse.
Once collected, the sample is sent to the laboratory for analysis, where technicians examine it under a microscope to evaluate the sperm count, motility, and morphology. The analysis will also assess the semen pH, the viscosity of the semen, and the time to liquefaction (the rate at which the semen changes from a sticky substance to a liquid).
After the test, a healthcare professional will explain the results to the patient and discuss the next steps.
Semen Sample Collection
Masturbation is the most common method for collecting a semen or sperm sample. However, some clinics may offer a special condom or, for individuals with severe male infertility, offer assistance with microsurgical epididymal sperm aspiration (MESA) or testicular sperm aspiration (TESA).
For accurate results, it’s important to abstain from ejaculation for two to seven days before the semen analysis. Additionally, specialists recommend patients avoid lubricants or saliva during collection as they can affect the quality of the sperm.
Key points to remember when preparing for a semen analysis
- Not all semen analysis labs are created equal. When selecting a lab, select an organization that is widely recognized for its credibility and trusted by both patients and healthcare professionals. Labs associated with fertility centers may be a good option as they have more experience analyzing semen samples.
- Semen quality varies with the collection technique; follow the directions exactly to ensure accurate results.
- Clean or sterile containers must be used to prevent sample contamination.
- Test results often vary, so patients may be asked to undergo multiple tests.
- Individuals who collect samples at home should ensure that they are kept at the correct temperature (usually at body temperature) during transport and submit them to the lab within one hour of collection.
How to Prepare for a Semen Analysis
Preparing for a semen analysis is relatively simple. Patients should abstain from sexual activity that results in ejaculation for two to seven days before sperm collection. This includes intercourse and masturbation. Patients should also ensure that their hands are clean and that they’ve wiped their genital area thoroughly (or showered) before collection.
A Word on At-Home Semen Analysis Kits
At-home semen analysis kits are available online or at select pharmacies, offering a convenient and cost-effective alternative to traditional laboratory testing. However, convenient as they are, these kits may not provide a level of accuracy comparable to that of a professionally administered test.
Furthermore, at-home tests may not detect underlying male fertility conditions, such as infections, hormonal imbalances, or genetic abnormalities.
For these reasons, healthcare professionals generally recommend a clinical semen analysis to diagnose male infertility accurately.
Understanding Semen Analysis Results
During a semen analysis, three primary factors are examined: the quantity of sperm (volume), the movement of the sperm (motility), and the shape of the sperm (morphology). These factors help to determine whether the semen parameters are within the reference range for male fertility.
This section aims to help patients decipher their semen analysis results.
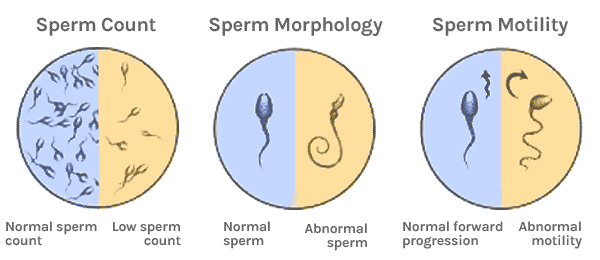
Understanding Sperm Count
Sperm count measures the total number of sperm cells in a semen sample (one ejaculate). The average sperm count ranges from 40 million to 300 million sperm per milliliter.
According to the World Health Organization (WHO), a “normal” sperm concentration is 15 million or more sperm per milliliter of semen.
If a patient’s sperm count is low, it may indicate infertility or reduced fertility. Individuals with no sperm in their semen may have a condition known as azoospermia.
A low sperm count (oligospermia) doesn’t mean conception is impossible. It just makes it more challenging and may require more advanced fertility treatments. In contrast, an abnormally high sperm count doesn’t guarantee fertility.
Sperm count is just one of the many factors contributing to male infertility that should be interpreted in conjunction with other semen analysis parameters and lifestyle factors that may affect fertility.
Understanding Sperm Motility
Sperm motility refers to the percentage of sperm that are actively moving. Being able to “swim” is a crucial aspect of sperm function, as that’s how they make their way to the egg for fertilization. When talking about motility, specialists evaluate sperm motility in two types of movement: total motility and progressive motility.
Total motility refers to the percentage of sperm that are moving, regardless of whether their movement is progressive or non-progressive. Progressive motility, on the other hand, refers to the percentage of sperm that are moving forward in a straight line or a circle.
For sperm to reach the egg successfully, they must have progressive motility of at least 25 micrometers a second. When less than 32% of the sperm cannot move efficiently, it may indicate low motility, also known as asthenozoospermia.
Understanding Sperm Morphology
Sperm morphology refers to the shape and size of sperm cells. These cells are classified as either “normal” or “abnormal” based on specific criteria. Many fertility clinics follow Kruger’s Strict Morphology guidelines to determine sperm morphology.
According to the Kruger criteria, “normal” sperm have an oval-shaped head, a straight tail, and no visible abnormalities. Sperm that deviate from these criteria are classified as abnormal. If the percentage of normal sperm is below 4%, the individual may have poor sperm morphology or teratozoospermia.
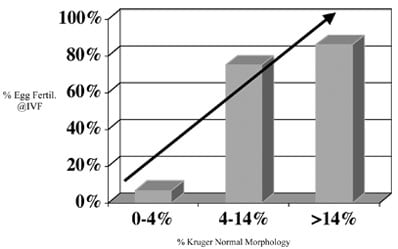
Sperm defects can vary in size, shape, and structure, including abnormalities in the neck, tail, and size. While some defects can harm sperm function, others do not. Couples with low sperm morphology may require IVF with intracytoplasmic sperm injection (ICSI), while couples with slightly abnormal scores may consider intrauterine insemination (IUI) treatment.
Although sperm morphology has been suggested as a marker for male fertility, not all experts agree on its significance in predicting fertility. Some studies have found that morphology is less accurate in predicting fertility than other semen parameters, such as motility and count.
How to Analyze a Semen Analysis Report
Reading the results of a semen analysis report can be overwhelming for many individuals, but understanding what each parameter means can help.
Here’s a guide to analyzing a semen analysis report:
- Check the date and time. Ensure the report is current and the analysis was conducted within the recommended time frame, generally within one hour of ejaculation.
- Look at the volume. This refers to the total amount of semen the individual produces during ejaculation and is typically measured in milliliters (ml). The World Health Organization (WHO) considers a volume of 1.5 ml or more to be normal.
- Check the sperm concentration. This refers to the number of sperm present in each milliliter of semen and is typically measured in millions per milliliter (m/mL). It should be 15 million or more per ml.
- Examine sperm motility. This refers to the percentage of sperm actively moving and is evaluated in total and progressive motility. As mentioned earlier, the minimum requirement for progressive motility is 25 micrometers per second.
- Assess sperm morphology. This refers to the size and shape of sperm and is evaluated according to specific criteria, such as Kruger’s Strict Morphology guidelines. The percentage of normal sperm should be above 4%.
- Look at other parameters. The report may also provide information on other factors, such as pH level, viscosity, and the presence of white or red blood cells.
Normal Semen Analysis Levels
| Areas of Review | Normal Semen Analysis Ranges |
| Total sperm count | 39 – 928 million |
| Ejaculate Volume | 1.5 – 7.6 mL |
| Sperm Concentration | 15 – 259 million per mL |
| Total Motility (progressive and non-progressive) | 40% – 81% |
| Progressive Motility | 32% – 75% |
| Sperm Morphology | 4% – 48% |
In short, healthy semen analysis reports include:
- active sperm
- a normal sperm count
- a pH balance within the normal range (low acidity, but not too alkaline)
- liquefaction of semen in 15 to 20 minutes
Abnormal Semen Analysis Results: What does it mean?
It’s important to note that a semen analysis report is just one tool used to evaluate male fertility, and a single abnormal result doesn’t necessarily mean that an individual is infertile.
Many factors can affect semen quality, and it’s not uncommon for semen analysis results to vary from one test to another. If the semen analysis report shows abnormal results, scheduling a follow-up appointment with a healthcare professional to discuss the results is important.

Additional Sperm Testing Options
Additional testing may be necessary to rule out underlying medical conditions, infection, or hormone abnormalities. This section outlines other sperm testing options.
Semen Leukocyte Analysis
This test measures the number of white blood cells in a semen sample. High levels of white blood cells, also known as leukocytes, in semen may indicate an infection or inflammation in the reproductive tract.
Karyotyping
Karyotyping is a genetic test that looks for chromosomal abnormalities in men with abnormal semen analyses. This test is usually recommended for individuals with a low or absent sperm count, as chromosomal abnormalities can cause this condition. Karyotyping can identify genetic disorders that the parents can pass on to their offspring.
Sperm Penetration Assay
The sperm penetration assay, also known as the hamster egg test, is a test that measures the ability of sperm to penetrate and fertilize an egg in a laboratory setting. Doctors often recommend this test for couples undergoing assisted reproductive techniques such as IVF to assess the fertilizing potential of sperm.
Anti-Sperm Antibody Test
The anti-sperm antibody test checks for antibodies that damage sperm. High levels of these antibodies can affect sperm movement and reduce fertility. The test can identify the cause of infertility and guide treatment.
Semen Analysis: In Conclusion
A semen analysis can help piece together the puzzle of male fertility, but it’s important to remember that it’s just one part of the evaluation process. If you or your partner receive abnormal results, don’t panic! Take a deep breath and schedule a follow-up appointment with your healthcare professional to discuss the results and create a plan.
Remember, infertility is an emotional and challenging journey, but many treatment options are available.
If you have concerns about your fertility, the experienced team at RMA Network can provide guidance and support. Our fertility specialists are dedicated to providing personalized care and creating treatment plans tailored to each patient’s unique needs. Make the first step and schedule an appointment today.
A Word from RMA: Reproductive Medicine Associates
At RMA: Reproductive Medicine Associates, we understand how overwhelming infertility can be. Our team is here to guide you through the diagnostic process and help you achieve your dreams of parenthood. Contact us today to schedule a consultation.





