Executive Summary
This article provides an in‑depth explanation of Anti‑Müllerian Hormone (AMH) testing and its vital role in evaluating ovarian reserve and guiding fertility care. AMH is a hormone produced by the cells surrounding developing follicles in the ovaries, and its levels—measured through a simple blood test—reflect the estimated number of eggs remaining. Because AMH directly correlates with egg quantity rather than egg quality, it offers valuable insight into reproductive potential without determining the likelihood of conception. Clinicians use AMH values alongside other fertility markers, such as follicle-stimulating hormone (FSH) and antral follicle count (AFC), to personalize IVF stimulation protocols, adjust medication doses, and optimize fertility treatment outcomes.
AMH levels naturally decline with age and can fluctuate based on individual factors like genetics, health, and conditions such as polycystic ovary syndrome (PCOS), where levels may appear elevated. While AMH testing is not a standalone predictor of fertility, it plays a critical role in fertility planning, helping patients and providers make informed decisions about family building, treatment timing, and fertility preservation options such as egg freezing. By understanding what AMH reveals—and what it does not—patients can approach their reproductive journey with greater clarity and confidence.
Anti‑Müllerian Hormone (AMH) Testing & Evaluating Ovarian Reserve
Before we talk about what an AMH test is, I think it is important for women to understand the basics of female fertility.
Women are born with all of the eggs they will ever have (approximately 1-2 million at birth). Throughout their lifespan, starting at the first menstrual cycle, the body recruits a group of follicles (each with a small immature egg inside) that have the potential to respond to hormones, grow, and ovulate.
Usually, a woman ovulates one egg per month. The eggs that do not get selected to ovulate dissolve, and the process repeats itself if a woman is not pregnant that month.
The average age of a woman having children in the US has been on the rise over the past few decades. As more women choose to advance their education and careers, they are delaying building a family. The result is that more women in their 30s and 40s are deciding to have children than in the past.
However, we know fertility declines as we age, so it’s important that women understand their fertility and what the current tests and treatments can and can’t do for them.
Only when women are armed with all of the knowledge will they be able to make informed decisions about their health!
What are AMH Levels in Fertility?
Anti-Müllerian Hormone (AMH) is a hormone produced by small follicles in a woman’s ovaries and is commonly measured through a simple blood test. Doctors often use AMH levels to estimate a woman’s ovarian reserve, which refers to the number of eggs she has remaining. While AMH doesn’t indicate egg quality, it gives helpful insight into overall fertility potential and can guide decisions around family planning or fertility treatments.
The nitty-gritty details about AMH
- AMH, or anti-mullerian hormone, is a substance granulosa cells produce in ovarian follicles.
- It is first made in primary follicles that advance from the primordial follicle stage. At these stages, follicles are microscopic and cannot be seen by ultrasound.
- AMH production is highest in preantral and small antral stages (less than 4mm diameter) of development.
- Production decreases and then stops as follicles grow. Almost no AMH is made in follicles over 8mm.
- Therefore, the levels are fairly constant, and AMH testing can occur any day during the woman’s cycle.
What does AMH mean regarding your fertility?
AMH is an important fertility test about a woman’s ovarian reserve today. Higher AMH values (greater than 1 ng/mL) usually signify a woman has a normal ovarian reserve. Lower numbers (less than 1 ng/mL) may indicate a woman with diminished ovarian reserve (DOR).
We know that a woman’s fertility declines as she ages, so we typically see AMH values decline as women age. The value of this test is that a woman with a low AMH can choose to improve her fertility now if she desires a family in the future.
Struggling to Conceive? This Guide Changes Everything
Discover the expert strategies to finally start your family—download your free guide by Dr. Marcy Maguire now!

How can an AMH blood test help diagnose infertility?
Since AMH is produced only in small ovarian follicles, blood levels of this substance have been used to attempt to measure the size of the pool of growing follicles in women.
- Research shows that the size of the pool of growing follicles is heavily influenced by the size of the pool of remaining primordial follicles (microscopic follicles in “deep sleep”).
- Therefore, a fertility doctor can determine the size of the remaining egg supply—or “ovarian reserve,” by reading the levels of an AMH blood test.
With increasing female age, the size of their pool of remaining microscopic follicles decreases. Likewise, their blood AMH levels and the number of ovarian antral follicles visible on ultrasound also decrease.
Women with many small follicles, such as those with polycystic ovaries (PCOS), have high AMH hormone values. Women who have few remaining follicles and those who are close to menopause have low anti-mullerian hormone levels.
What does AMH measure?
What AMH is:
A great tool to assess a woman’s current ovarian reserve. It gives an overall picture of what you look like today.
Additionally, it can help set realistic expectations on the number of eggs that may be retrieved. It can also indicate how you will respond to medication should you decide to proceed with IVF, either for infertility or for egg freezing.
What AMH is not:
A predictor of whether a woman can get pregnant spontaneously in the future.
The only true test of whether a woman can conceive, regardless of her AMH values, is for her to get pregnant on her own. A large cohort study demonstrated that there was NO difference in pregnancy rates in women with normal AMH values trying to conceive versus women with low AMH levels (less than 1 ng/mL) trying to conceive.
If you check your AMH today and get a low number, that does not mean you can’t get pregnant tomorrow or in 3 months if you were to try on your own.
Just because you have “normal” AMH levels currently does not predict that it will stay normal in the future. All women will have a decline in fertility as they age; how rapidly that decline occurs is different for every woman and can’t be predicted.
Should I get an AMH test?
I am a big proponent of women being educated about their fertility so they feel empowered to make decisions regarding their health. One part of that education is knowing what your ovarian reserve looks like at a given time and, once you have that information, what, if anything, you want to do about it.
AMH values can help you determine if you want to do something NOW for your fertility. Remember, AMH tells you what your ovarian reserve is now. They can’t predict how quickly your ovarian reserve will decline in the future, and they can’t predict if you will be able to get pregnant spontaneously on your own.
What is a normal AMH level? What is a low AMH level range?
AMH levels, measured in ng/mL, help estimate a woman’s ovarian reserve. A normal range is typically between 1.0 and 3.0 ng/mL, indicating a healthy egg supply for age. Levels below 1.0 ng/mL are considered low and may suggest diminished ovarian reserve, while levels above 3.0 ng/mL are often seen in women with polycystic ovary syndrome (PCOS) and may indicate a higher egg count. Though AMH reflects egg quantity, it does not measure egg quality and should be considered alongside other fertility factors.
Interpretation of anti-mullerian hormone levels
There are some inconsistencies to consider when interpreting an AMH blood test results. Since the AMH test has not been in routine use for many years, the levels considered to be “normal” have not yet been clarified and agreed upon by the experts. Also, not all current commercial assays give equivalent results.
The table below has AMH interpretation guidelines from fertility literature. Please review your AMH result with your fertility doctors. The graph below should only act as a guide.
For example, the difference between 0.6 and a 0.7 ng/ml test result puts a woman in a “different box” in this table. In reality, there is very little real difference in fertility potential. In reality, it is a continuum – and not something that categorizes well.
It is possible to have undetectable AMH levels if the values are extremely low.
|
Interpretation |
AMH Blood Level |
| Very High AMH Levels (often an indicator of PCOS) | Over 3.0 ng/ml |
| Normal AMH Levels | Over 1.0 ng/ml |
| Low Normal AMH Levels | 0.7 – 0.9 ng/ml |
| Low AMH Levels | 0.3 – 0.6 ng/ml |
| Very Low AMH Levels | Less than 0.3 ng/ml |
The below graph shows the average AMH level for women not experiencing trouble conceiving, according to age.
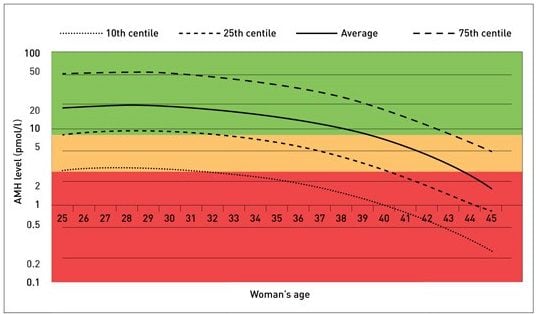
PLEASE NOTE: The above table, AMH Blood Levels (by ng/ml) should not be compared to the graph below (measured by pmol/l) as they are measured in different increments.
More will be learned regarding anti-mullerian hormone levels and outcomes. We continue to use the AMH fertility test and study the relationship between AMH hormone values, fertility, and ovarian responsiveness.
Can AMH Levels Fluctuate?
Recent studies have shown that significant fluctuations can be seen for several conditions and should be considered when interpreting AMH results. However, menstrual cycle fluctuations were minor, meaning AMH can be measured independently of the cycle phase.
Does insurance cover an AMH test?
Some insurance companies will cover the testing of AMH as a basic diagnostic test.
The best way to find out is to speak to your insurance provider or physician. Otherwise, you can pay cash, and that price will vary based on the clinic or lab you use.
Testing for a single AMH test can range from $20 to slightly higher. Each RMA office accepts different insurance plans.
Treatment Options for Low AMH Levels
The most beneficial treatment for low AMH is in vitro fertilization (IVF).
Depending on your diagnosis, your physician will either recommend an IVF with your own eggs or through the use of donor eggs.
Having low AMH levels means that you have a low egg reserve, which is why it is more difficult to get pregnant, but this does not mean that you can not get pregnant naturally. It only takes one healthy egg to become pregnant. It does mean that you may have a very difficult time achieving a pregnancy on your own.
AMH levels increase and decrease slightly from one cycle to another, so you may be considered low in one cycle and very low in another.
Living a healthy lifestyle and getting the necessary nutrients such as Vitamin D may also increase your AMH levels. You can learn more about fertility supplements here.
What questions should women ask their doctors about AMH levels?
Women should talk to their doctors about ordering an AMH if they are interested in learning about their fertility and where it stands now.
If you find out you have a lower-than-expected AMH, you should consider consulting with a fertility doctor to discuss the options of egg freezing if you are not ready to start a family now.
AMH Levels for IVF
Women with higher AMH values will tend to respond better to ovarian stimulation for IVF (in vitro fertilization), with more eggs retrieved. Women with lower AMH have lower antral follicular counts and produce fewer oocytes (eggs).
AMH levels probably do not reflect egg quality. Having more eggs at the IVF egg retrieval allows a greater number of eggs to fertilize and develop into embryos. More eggs do not always mean more embryos. Egg quality plays a role in the fertilization and development of embryos. The ultimate goal is to have at least one healthy embryo to transfer back into the uterus.
How to Increase AMH Levels
A low AMH level means a woman has a low ovarian reserve (egg supply).
Low AMH means that you have a low ovarian reserve, but it doesn’t mean that you are unable to conceive naturally. Unfortunately, there are no proven ways to increase your AMH levels. Although, some research has shown that vitamin D and DHEA may help increase AMH levels.
Ovarian reserve testing methods
The anti-mullerian hormone is just one potential test of ovarian reserve. Fertility specialists often use a combination of fertility tests to assess a woman’s ovarian reserve best. These tests include a transvaginal ultrasound to count the number of antral follicles and blood tests to determine hormone levels.

How Do FSH and AMH Levels Affect Pregnancy?
Dr. Marcy Maguire, one of RMA’s reproductive endocrinologists, recently explained FSH and AMH in detail on an episode of This is Infertility, a new podcast examining what it’s like to be infertile in the U.S.
Frequently Asked Questions about AMH Testing
What is premature ovarian aging, premature ovarian insufficiency, or diminished ovarian reserve?
All of the above terms for premature ovarian aging mean essentially the same thing: the ovaries have fewer eggs in them than they should, given the woman’s age. Diminished ovarian reserve is not synonymous with whole-body aging – it doesn’t mean that the woman herself is somehow aging prematurely; it just means her egg count overall is lower than it should be given her age.
What are the symptoms of premature ovarian aging?
The two most common symptoms are infertility and irregular or skipped menstrual cycles.
How can a fertility specialist diagnose premature ovarian aging?
The best diagnosis will come from FSH and AMH levels and then an ultrasound – all three can be markers of a lower egg count.
What is FSH?
FSH, or follicle-stimulating hormone, is a hormone produced by the pituitary. The pituitary is an organ in the brain that encourages follicles and eggs to grow and mature each month. If the FSH level starts to go up, typically above the number often, that means that the brain is trying hard to stimulate the ovaries to produce eggs but is having a hard time getting the ovaries to listen. When FSH levels increase they are essentially getting louder to tell the ovaries to listen. Since there aren’t many eggs left, the ovaries are having a harder time producing.
What is AMH?
Anti-Mullerian is a hormone that is made by granulosa cells that take care of a woman’s eggs. The more eggs a woman has, the more granulosa cells she has and the higher her AMH. We like to use AMH as a marker of a woman’s overall egg count. If the AMH is above 1.2, we feel relatively reassured. If the AMH level is less than 1.2, that is more concerning. Of course, this will also correlate with a woman’s age, so a woman in her early 30s with a low AMH of less than 1.2 is very worrisome, whereas it’s more common for women in their early 40s to have a low AMH.
How do you test for FSH and AMH?
A blood test will identify a woman’s FSH and AMH levels.
What are fertility options for women with high FSH and low AMH?
If a woman has diminished ovarian reserve, meaning an overall lower egg count, she still may have the opportunity to have children using her own eggs – it just depends on her relative level of eggs. If there are some that we can access, we would typically do in vitro fertilization (IVF) to retrieve them. A woman could also potentially bank some of the eggs retrieved. Eggs that are banked are then cryopreserved or “frozen and can be used in future IVF cycles.
What if a woman cannot use her own eggs at all?
When a woman’s egg reserve is so low that she is in the early stages of menopause, fertility treatments typically can’t help a woman use her own eggs – but donor eggs (from both known and anonymous donors) are available, and the woman can carry the pregnancy herself.
RESOURCES: ReprodcutiveFACTS.org





