Reproductive Medicine Associates of New Jersey (RMANJ) third year fellow Dr. Shelby Neal has received the American Society for Reproductive Medicine (ASRM) Corporate Member Council In-Training Travel Award for her research on the link between adenomyosis seen on 3D ultrasound and clinical outcomes following IVF.
Dr. Neal’s research showed that only women with obvious adenomyosis on 3D ultrasound are at increased risk for adverse outcomes following Frozen Embryo Transfer (FET). Specifically, the study demonstrates that women with obvious adenomyosis have a higher likelihood of experiencing miscarriage.
“Most of the prior studies regarding adenomyosis focused on outcomes following fresh embryo transfer,” Dr. Neal said. “With an increasing trend toward frozen embryo transfer, we felt it was important to examine outcomes in this patient population.”
Diagnosing Adenomyosis
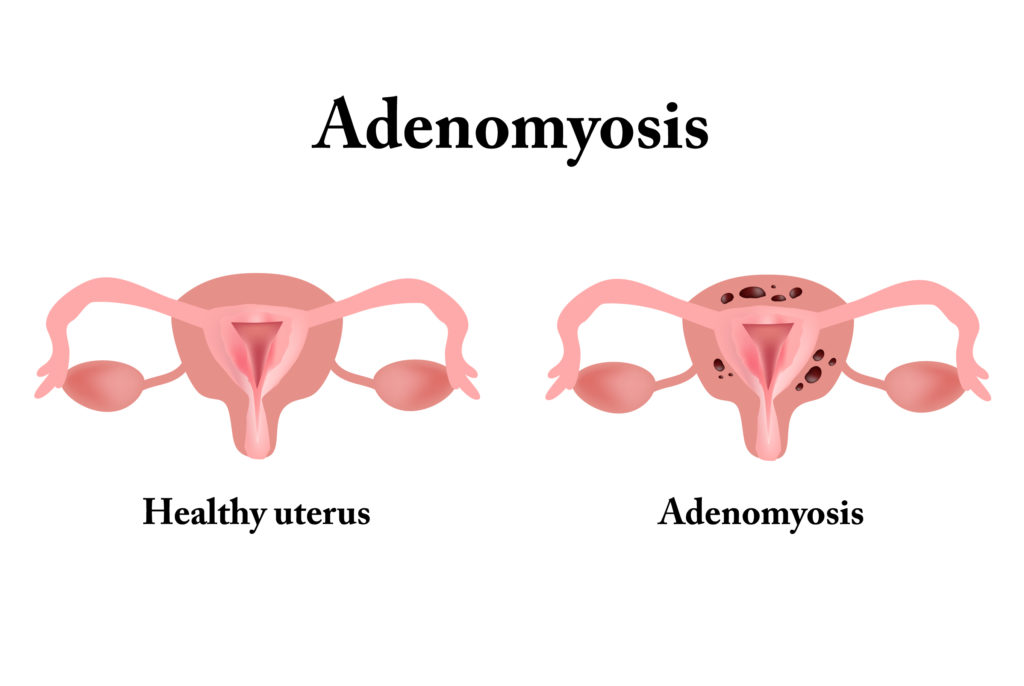
Adenomyosis, a condition marked by the growth of endometrial tissue into the walls of the uterus, can cause pelvic pain, irregular bleeding and infertility. Diagnosis of the condition has traditionally required examination of a hysterectomy specimen. However, hysterectomy is not practical for patients desiring to conceive, resulting in exploration of less invasive ways to diagnose it.
Enter 3D ultrasound, which enables doctors to non-invasively image the uterus and identify markers of adenomyosis in a matter of seconds. In addition to identifying those markers, 3D ultrasound has the ability to image the external contours of the uterus as well as the size and shape of the uterine cavity. Because the interpretation of the imaging can be subjective, further research was necessary to understand the predictive value of adenomyosis diagnosed on 3D ultrasound with respect to clinical outcomes following IVF.
So Dr. Shelby Neal, along with colleagues Dr. Linnea Goodman, Dr. Scott Morin, Dr. Marie Werner, and Dr. Ndeye-Aicha Gueye, undertook a prospective observational study to learn more. Between April and December last year, over 700 existing RMANJ patients took part in the study by consenting to undergo a 3D ultrasound on the day before their FET. The images were reviewed by all five of the doctors and evaluated for seven markers of adenomyosis. Once participating patients had achieved a clinical outcome, those were logged, and the data was analyzed.
Clinical Outcomes
Dr. Neal began by evaluating outcomes in patients with adenomyosis (diagnosed by at least 3 out of 5 doctors) compared to those without adenomyosis and found no difference in clinical outcomes. However, when looking at the 21 patients with obvious adenomyosis – those patients for whom all five reviewing physicians identified adenomyosis – some differences began to emerge. Specifically, patients with obvious adenomyosis were almost four times as likely to experience a miscarriage compared to those without adenomyosis – those with the condition had a 23.8 percent chance of miscarrying while those without it had a 6.3 percent chance.
“What was probably most interesting, however,” Dr. Neal said, “is that we did not see a difference in clinical outcomes for patients with more subtle adenomyosis, suggesting that only patients with obvious adenomyosis are at increased risk for adverse outcomes following frozen embryo transfer.”
Dr. Neal said that more research is needed to identify which ultrasound markers of adenomyosis are most predictive of adverse outcomes and to evaluate potential treatments to optimize outcomes in this population.
MAKE AN APPOINTMENT




